Most people know their “Total Cholesterol” number, but Triglycerides—the most common type of fat in your body—often go ignored until they reach a dangerous threshold. Unlike a fever or a rash, high triglycerides are often “silent,” showing no symptoms until they trigger a major medical event like a heart attack or acute pancreatitis. At 6CPC, we believe that understanding these markers is the first step toward Control and Care.
Chapter 1: The Biology of Lipids – What are Triglycerides?
To understand the danger, one must first understand the molecule. Triglycerides are a type of lipid (fat) found in your blood. When you eat, your body converts any calories it doesn’t need to use right away into triglycerides. The triglycerides are stored in your fat cells. Later, hormones release triglycerides for energy between meals.
The Chemical Structure
Chemically, a triglyceride is an ester derived from glycerol and three fatty acids. This structure is why they are called “tri-” glycerides. They are the main constituents of body fat in humans and other vertebrates, as well as vegetable fat.
Triglycerides vs. Cholesterol
People often confuse the two. Here is the distinction:
Triglycerides store unused calories and provide your body with energy.
Cholesterol is used to build cells and certain hormones. Because neither can dissolve in blood, they circulate through your body with the help of proteins that transport the lipids (lipoproteins).
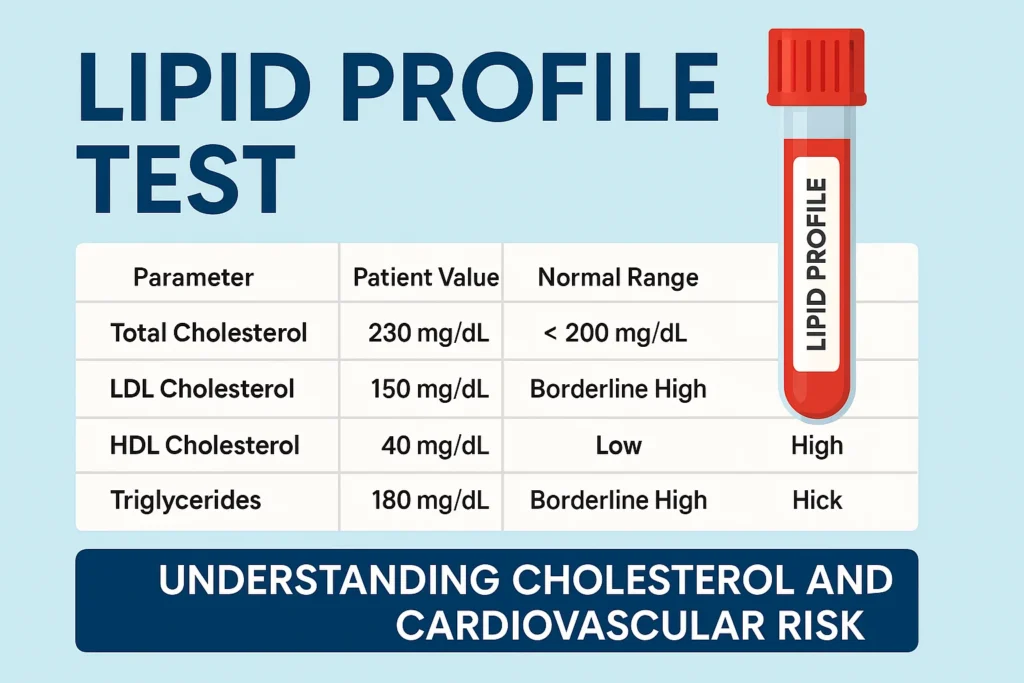
Chapter 2: The "Silent" Scale – Interpreting Your Lipid Profile
A blood test (Lipid Panel) measures your triglycerides along with your HDL (good) and LDL (bad) cholesterol. At 6CPC, we emphasize knowing your numbers. Triglycerides are lipids (fats) that circulate in your blood. When you eat, your body converts any calories it doesn’t need to use right away into triglycerides, which are stored in your fat cells. Later, hormones release them for energy between meals. However, when you consistently consume more calories than you burn—particularly from high-carb or sugary foods—your levels can skyrocket.
The Clinical Ranges
Normal: Less than 150 milligrams per deciliter (mg/dL).
Borderline High: 150 to 199 mg/dL.
High: 200 to 499 mg/dL
Very High (Severely Elevated): 500 mg/dL or higher.
When to Test?
The American Heart Association recommends that all adults 20 or older have their cholesterol and other risk factors checked every four to six years. If you have a family history of heart disease, you should test annually.
Chapter 3: The Danger Zones – Hypertriglyceridemia and the Pancreas
When triglycerides exceed 500 mg/dL, the risk moves beyond the heart to pancreas. Extremely high levels can cause Acute Pancreatitis—a sudden, severe inflammation of the pancreas that is a medical emergency.
Signs of Emergency: If you have high triglycerides and experience sudden, intense abdominal pain that radiates to your back, nausea, or vomiting, seek help immediately at a facility like KIMSHEALTH Nagercoil or your nearest speciality hospitals.
Understanding Acute Pancreatitis
Acute pancreatitis is a sudden inflammation of the pancreas. High levels of triglycerides in the blood can cause the release of free fatty acids, which are toxic to the pancreatic cells.
Symptoms: Severe upper abdominal pain that radiates to the back, tenderness when touching the abdomen, fever, rapid pulse, and vomiting.
The Emergency Factor: This condition can lead to multi-organ failure. If you experience these symptoms, emergency care is vital.
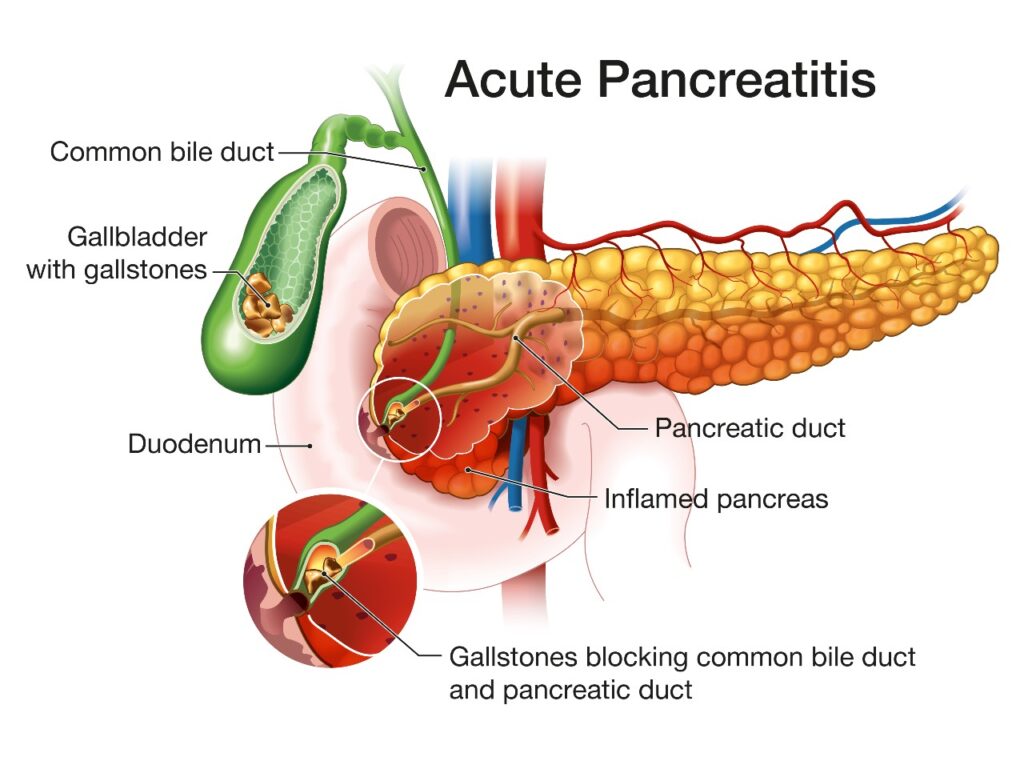
The Pancreatitis Connection – A Deep Dive into Hypertriglyceridemic Pancreatitis (HTGP)
When we discuss high triglycerides at 6CPC, we aren’t just talking about long-term heart disease. We are talking about a potential acute crisis. Hypertriglyceridemic Pancreatitis (HTGP) is the third most common cause of acute pancreatitis, following alcohol and gallstones, accounting for up to 10% of all cases.
The Pathophysiology: Why Fat Inflames the Pancreas
The pancreas is a delicate organ responsible for producing digestive enzymes and insulin. Under normal conditions, triglycerides circulate in the blood packaged in large particles called chylomicrons. However, when triglyceride levels exceed 1,000 mg/dL (and sometimes as low as 500 mg/dL), the concentration of these particles becomes so high that they “clog” the tiny capillaries of the pancreas. This lead to:
Ischemia: Reduced blood flow to the pancreatic tissue.
Lipolysis: The enzyme pancreatic lipase begins to break down these excess triglycerides prematurely, releasing Toxic Free Fatty Acids.
Chemical Burn: These fatty acids act like a chemical irritant, damaging the cell membranes of the pancreas and triggering an inflammatory “storm.”
Recognizing the Clinical Stages of HTGP
Understanding the progression of symptoms can be life-saving. Medical professionals typically categorize the onset into three stages:
Stage 1: The Prodromal Phase (The Warning)
Before the full-blown attack, many patients report a “heavy” feeling in the upper abdomen. This is often accompanied by:
Xanthomas: Small, yellowish skin bumps (fatty deposits) usually appearing on the back, buttocks, or limbs.
Lipemia Retinalis: A milky appearance of the retinal veins (visible only during an eye exam).
Stage 2: The Acute Attack
This is the “emergency” phase. The pain is usually described as “boring” or “tearing.”
Location: Pain starts in the epigastric region (just below the ribs) and radiates straight through to the back in 50% of cases.
The “Leaning Forward” Sign: Many patients find slight relief only by leaning forward or curling into a fetal position.
Systemic Response: High fever, rapid heart rate (tachycardia), and shallow, rapid breathing.
Stage 3: The Complication Phase
If the inflammation isn’t controlled, it can lead to:
Pancreatic Necrosis: Tissue death within the organ.
Pseudocysts: Fluid-filled sacs that can rupture or become infected.
Organ Failure: Specifically affecting the lungs (ARDS) and kidneys.
Diagnostic Criteria: What the Doctors Look For
When you arrive at a hospital like KIMSHEALTH Nagercoil, doctors will use the Atlanta Criteria to diagnose you. This requires two of the following three:
Characteristic abdominal pain.
Serum amylase or lipase levels at least three times the upper limit of normal.
Findings of acute pancreatitis on imaging (CT scan or MRI).
The 6CPC Treatment Protocol: From Hospital to Home
In the hospital, the primary goal is “pancreatic rest.”
NPO (Nothing by Mouth): To stop the pancreas from producing digestive enzymes.
Intravenous Insulin: Interestingly, insulin helps activate lipoprotein lipase, an enzyme that clears triglycerides from the blood.
Plasmapheresis: In extreme cases, the patient’s blood is filtered to physically remove the excess fat.
Transitioning to Long-Term “Care”
Once the acute phase passes, the focus shifts back to the 6CPC Pillars. You must transition to a strictly low-fat diet (less than 20g of fat per day initially) and begin a regimen of fibrates or high-dose Omega-3s as prescribed.
Chapter 4: Hemodynamics – The Link Between Lipids and MAP
This is where our 6CPC Mean Arterial Pressure (MAP) Calculator becomes essential. High triglycerides contribute to the thickening of the blood and the hardening of the arteries (atherosclerosis). High triglycerides contribute to atherosclerosis (hardening of the arteries). When your arterial walls thicken, your heart must work harder to pump blood, which directly impacts your Mean Arterial Pressure (MAP).
What is Perfusion?
Perfusion is the process of a body delivering blood to a capillary bed in its biological tissue. When your blood is “lipemic” (thick with fat), the resistance in your vessels increases.
The MAP Connection: Your Mean Arterial Pressure must remain in the 70–100 mmHg range to ensure that despite the arterial resistance caused by high triglycerides, your kidneys and brain are still getting blood.
Tool Tip: Use our Mean Arterial Pressure (MAP) Calculator to see if your heart is successfully perfusing your organs despite high lipid levels.
Chapter 5: Causes of Elevated Triglycerides
Why do these levels rise? It is rarely just one factor. when you consistently consume more calories than you burn—particularly from high-carb or sugary foods—your levels can skyrocket.
Obesity and Overweight: Excess weight is the most common cause.
Self-Correction: Use the BMI Calculator on our homepage to assess your risk category.
Poor Diet: Diets high in refined carbohydrates, sugar, and alcohol.
Physical Inactivity: A sedentary lifestyle prevents the body from “burning off” stored triglycerides.
Genetic Factors: Familial hypertriglyceridemia is a condition passed through families.
Medications: Certain diuretics, beta-blockers, and steroids can raise levels.
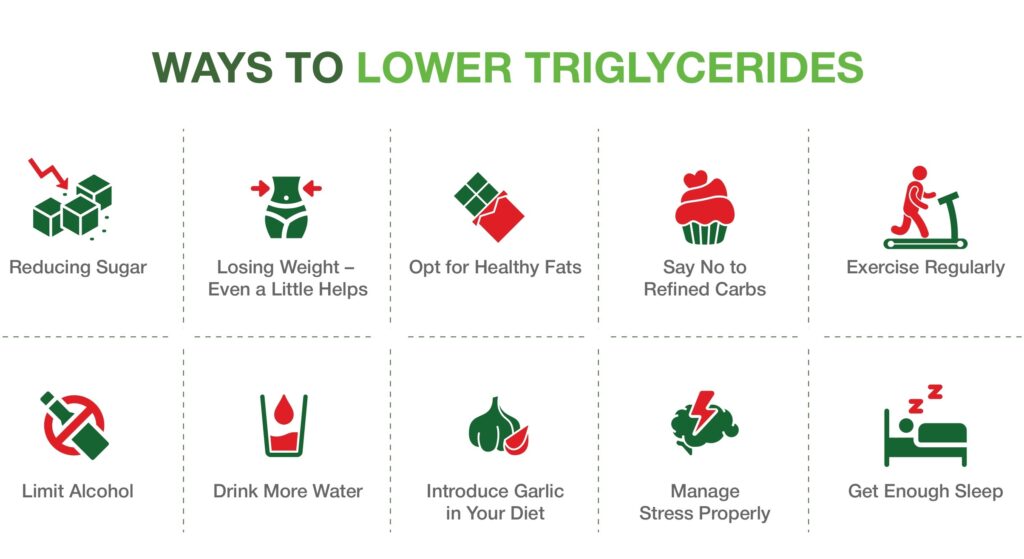
Chapter 6: The "Purify" Protocol – Natural and Clinical Management
To lower triglycerides, one must adopt a multi-faceted approach.
Dietary Overhaul
Eliminate Fructose: The liver converts fructose directly into triglycerides. Avoid sodas, corn syrup, and excessive fruit juice. Fructose is a primary driver of triglyceride production in the liver. Switch from sodas and processed juices to water or Immunity Boosting Tulsi Tea.
Omega-3 Fatty Acids: These are “power clearers” for the blood. Sources include salmon, mackerel, and flaxseeds.
The Power of Fiber: Soluble fiber (found in oats and beans) helps decrease the absorption of fat into the bloodstream.
Prioritize Healthy Fats: wap trans-fats for Omega-3 fatty acids found in walnuts, flaxseeds, and fatty fish. These fats help “clear” the triglycerides from your bloodstream.
Manage Your BMI: Weight loss is the most effective way to drop lipid levels. Even a 5-10% reduction in body weight can lead to a 20% drop in triglycerides. Check your current status with our BMI and Ideal Body Weight Calculator to set a realistic weight loss goal.
The Role of Ayurvedic Wisdom
Traditional remedies like Tulsi (Holy Basil) and Garlic have been shown in various studies to support metabolic health. Tulsi helps in reducing metabolic stress, which can indirectly help in managing lipid levels.
Chapter 7: Exercise Science – How Physical Movement "Cleanses" the Blood
If diet is about what you put into the “tank,” exercise is about how efficiently the engine burns the fuel. At 6CPC, we view exercise not just as a way to lose weight, but as a primary clinical intervention for lipid management.
1. The Role of Lipoprotein Lipase (LPL)
The secret to lowering triglycerides through movement lies in an enzyme called Lipoprotein Lipase (LPL). Think of LPL as a “gatekeeper” located on the walls of your blood vessels. Its job is to grab triglycerides as they float by in the bloodstream and break them down into free fatty acids that your muscles can use for fuel. When you are sedentary (sitting for long periods), LPL activity drops significantly. This causes triglycerides to linger in your blood, increasing your risk of plaque buildup. However, as soon as you start moving—even just walking—LPL activity is “switched on,” effectively vacuuming the fat out of your blood.
2. The Power of the “Post-Prandial” Walk
One of the most effective strategies for managing triglycerides is the Post-Prandial Walk (a walk taken immediately after a meal). When you eat a meal rich in fats or carbohydrates, your blood triglyceride levels peak about 2 to 4 hours later. By walking for just 15–20 minutes shortly after eating, you stimulate muscle contractions that demand energy. Your body responds by pulling those newly digested triglycerides out of the blood before they can be sent to storage in your fat cells.
3. Aerobic vs. Resistance Training: The Dual Approach
To reach optimal metabolic health, a combination of both types of exercise is required:
-
Steady-State Aerobic Exercise (Cardio): Activities like swimming, cycling, or brisk walking are the “gold standard” for triglyceride reduction. Long-duration cardio increases the number of mitochondria in your cells, which are the factories where fats are burned for energy.
-
Resistance Training (Weight Lifting): Muscle tissue is metabolically expensive—it burns energy even when you are resting. By increasing your muscle mass, you increase your body’s baseline demand for triglycerides, making it harder for your levels to spike.
4. The “Intensity” Factor and MAP
As you exercise, your heart rate increases, which directly impacts your Mean Arterial Pressure (MAP). Regular exercise strengthens the heart muscle, allowing it to pump more blood with less effort. Over time, this lowers your resting heart rate and stabilizes your MAP, ensuring that your organs are well-perfused without putting undue stress on your arterial walls.
Tool Tip: After a workout, once your heart rate has settled, use our MAP Calculator to see how your resting hemodynamics are improving over time.
Chapter 8: The Metabolic "Afterburn" (EPOC)
High-Intensity Interval Training (HIIT) creates a phenomenon known as Excess Post-exercise Oxygen Consumption (EPOC). After an intense workout, your body continues to burn calories (and triglycerides) at an elevated rate for up to 24 hours as it works to repair tissues and restore oxygen levels. For busy individuals, this “afterburn” is an efficient way to manage lipids with shorter workout durations.
Chapter 9: Practical Workout Plan for Triglyceride Control
| Phase | Activity Type | Duration | Frequency |
| Daily | Post-Meal Walk | 15 Minutes | 3x Daily |
| Aerobic | Brisk Walk or Cycling | 30–45 Minutes | 5x Weekly |
| Strength | Full Body Resistance | 20 Minutes | 2x Weekly |
Chapter10: Frequently Asked Questions (Deep Dive)
Q1. Can stress cause high triglycerides?
Answer: Yes, stress triggers the release of cortisol, which can increase blood sugar and subsequently triglycerides.
Q2. Is alcohol a factor?
Answer: Alcohol is very high in calories and sugar; it has a particularly potent effect on raising triglycerides.
Q3. What if diet isn’t enough?
Answer: In some cases, doctors prescribe fibrates, niacin, or prescription-strength fish oil.
Conclusion: The 6CPC Philosophy
Managing your health isn’t about fear; it’s about Control, Purify, and Care. By understanding the silent markers like triglycerides and using tools like our MAP and BMI calculators, you are taking the driver’s seat in your wellness journey.
